Retrieving Separate Payment for COVID-19 Vaccines

Client Overview:
Our client, a healthcare provider administering COVID-19 vaccines, faced reimbursement challenges when multiple insurance payers bundled vaccine payments with standard office visit charges. As a result, the client was not receiving separate reimbursement for vaccine administration.
Challenge
The practice encountered recurring reimbursement issues, including:
- Insurance plans bundling COVID-19 vaccine payments with office visit charges
- Denial of separate reimbursement for vaccine administration
- Revenue loss due to underpayment
- Lack of clarity and inconsistent interpretation of payer-specific COVID billing policies
These issues led to reduced reimbursement and financial discrepancies in the revenue cycle.
Solution
To resolve the issue and recover lost revenue, we implemented a focused reimbursement recovery strategy:
In-Depth Policy Review
Our team conducted a detailed review of:
CMS COVID-19 vaccine billing guidelines
Payer-specific reimbursement policies
Federal and state-level billing directives regarding vaccine administration
This helped us identify where payers were incorrectly bundling payments.
Strong Appeal Drafting
We prepared comprehensive appeal letters that:
Cited official COVID-19 billing guidelines
Referenced appropriate CPT codes and vaccine administration codes
Included supporting documentation to validate separate reimbursement eligibility
Persistent Follow-Up
Our billing specialists conducted proactive follow-ups with insurance carriers to ensure appeals were reviewed accurately and processed in a timely manner.
Results
Our strategic intervention produced measurable financial improvements:
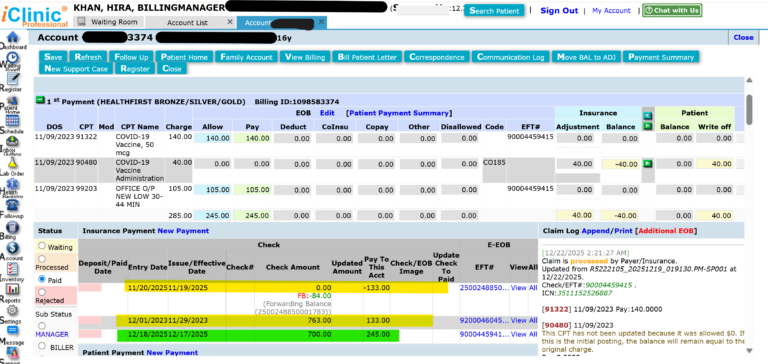
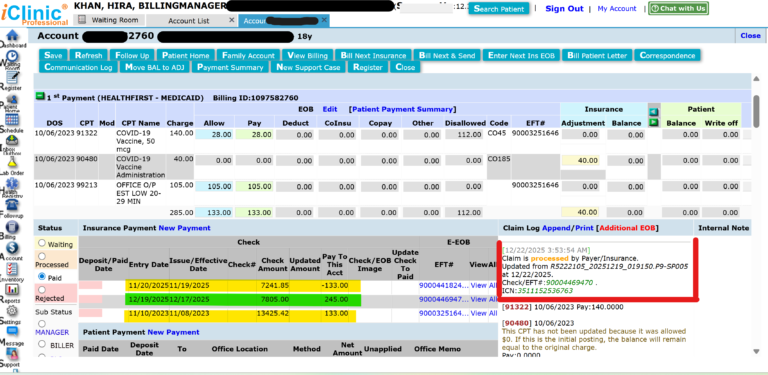
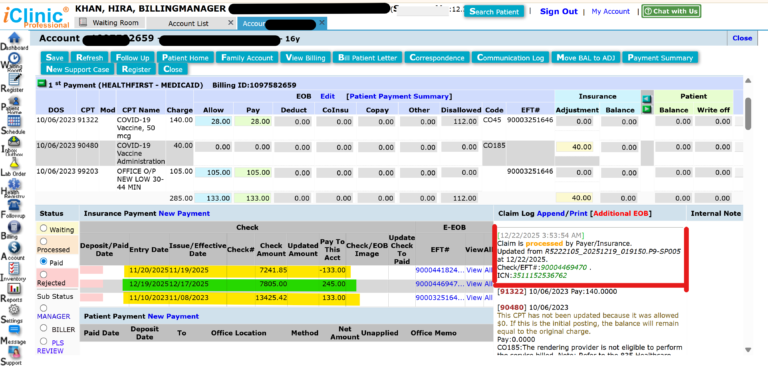
- Appeals were successfully approved
- Payers reprocessed claims and recouped initial payments
- Revenue leakage from improper bundling was effectively eliminated
- Providers received higher reimbursement rates, including separate payment for COVID-19 vaccine administration
Supporting Evidence